Introduction
'Show me the money’ is the infamous line from the hit movie Gerry Maguire. Well, that’s pretty easy when it comes to echinacea.
Echinacea ranks as one of the top selling herbs worldwide and grossed a staggering $15.1 million in 2008 alone. To put this in perspective, $15.1 million exceeds the national health budget of some countries.
This huge amount of money is spent on echinacea because it is purported to be useful for common colds, flus, respiratory tract infections and as an all-purpose immune booster.
We are still right in the middle of cold and flu season and before I can ask any of my patients to part with their hard earned money, I think it is reasonable to ask the question ‘Show me the research?’ to back up this incredible expenditure.
What Is Echinacea?

Echinacea are a group of native American wildflowers. Indigenous to North America, they were introduced into Germany in the 1920s.
They come from the daisy family (Asteraceae/Compositae) and are sometimes called coneflowers. Archaeological digs at the Lakota Sioux village site has found evidence of echinacea dating back to the 1600s. Native Americans used echinacea for a wide variety of cures. Echinacea was typically used for snake-bites, burns and coughs in indigenous cultures.
There are nine discrete species of echinacea with Echinacea purpurea (purple coneflower) as the most widely used species in North America. Other commonly used species include Echinacea pallida and Echinacea angustifolia.
Echinacea contains a number of classes of potentially bioactive compounds:
- alkamides,
- glycoproteins,
- polysaccharides
- cichoric
- caftaric and
- caffeic acid derivatives.
There is no consensus as to the key medicinal components of echinacea. The pharmacologic effects may be due to any of these parts independently or synergy between multiple constituents.
Additionally, variability occurs due to different species of echincea.
Just to complicate things further, the age and season of harvest, different parts (herb, root, flower, aerial parts, whole plant), different manufacturing methods (drying, alcoholic extraction or freshly pressed juice), addition of different plants, herbs or homeopathic remedies all contribute to variability in the constituents of any given echinacea product.
Doses recommended by herbalists, manufacturers and used in studies are 300-400mg of dried extract three times per day or one cup of tea (1 gram in 150 mL of boiling water for 5 minutes).
There are over 2000 echinacea products (tinctures, sprays, powder and tablets) for sale on Amazon and cost up to $6.25 per fluid ounce and $18.29 per ounce.
Let's divide that $15.1 million on echinacea sales by say a $10 average purchase price and we can see that there are lots of echinacea purchases every year.
Can You Get Echinacea From Food?
The answer to that question would be a 'no' (unless you have a thing for coneflower sandwiches).
Is There Any Research?
There are 1143 publications on echinacea which includes 86 clinical trials. To put this into context, Tamiflu has 3837 references and 137 clinical trials.
Does Echinacea Help Fight Cancer?
There are three studies that relate to cancer and echinacea.
The first paper is a pharmacokinetc study in one of my favorite journals - The British Journal of Clinical Pharmacology (1). The aim of the study was to evaluate the pharmacokinetics of the chemotherapy agent docetaxel in the presence of echinacea.
Ten patients received docetaxel (135 mg, 60 min IV infusion) before and after 14 days of echinacea (20 oral drops three times daily).
No clinically significant changes in the area under the curve, maximum concentration or half life of docetaxel were noted. An interesting but not very important study
Bottom line
Does It Boost Immune System?
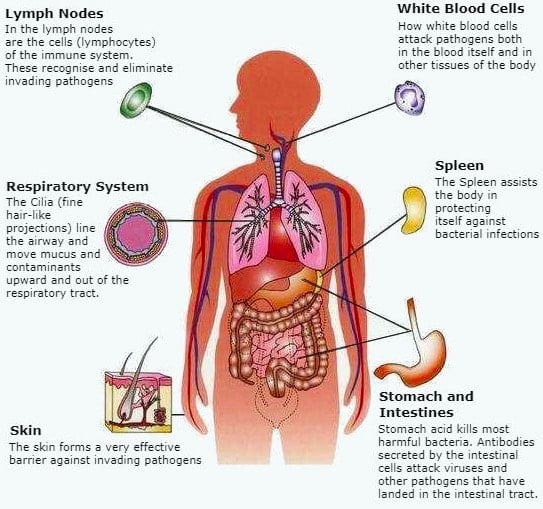
Gene expression analysis of over 13,000 genes showed that echinacea modulated the immune response and intracellular factors involved in multiple signalling pathways (4).
Another group of investigators noted that the main evidence base supporting echinacea as an immuno-modulator comes from either in vitro studies or use of echinacea as a parenteral agent (5).
These (smart) investigators were sceptical about the immuno-modulating effects of commoner gardener commercially available echinacea. They used a commercially available freshly pressed juice of echinacea in a study of 40 healthy volunteers.
The men were randomized to either echinacea or placebo for 2 weeks, followed by a four week wash-out period and they the men took either placebo or echinacea ( depending on which option that took during the first 14 days).
Echinacea had no effect on key parameters of immune function namely phagocytes, polymorhophonuclear leucocytes, monocytes, TNF- alpha and IL-1 beta. There was an unexplained finding of a statistically significant reduction in serum ferritin.
Ferritin is marker of iron stores but is also a marker of inflammation. The authors concluded that if echinacea has any immunomodulation effects that it must be mediated by effects other than those investigated in this study. Sounds like a cop out to me.
Other investigators found that echinacea supplementation increased white blood cell counts and expression of leucocyte heat shock protein 0 and had an anti-oxidant effect (6). However this was a non-randomized controlled pilot study in just 11 volunteer over 14 days.
Bottom line
There is essentially nothing in the medical literature to support a role for echinacea as a credible immune-modulator.
Does It Alleviate Pain?
There are only two studies that relate to echinacea and pain.
In the first study, a total of 15 patients who were non-responders to non steroidal anti-inflammatory drugs (NSAIDS) for pain due to knee arthritis were given a combination of ginger plus echinacea for 30 days (7). A statistically significant improvement in pain was noted compared to baseline in the study subjects.
The problems with the study include the fact that it was a small short term, non-randomized, non-placebo controlled trial and it is impossible to deconstruct the effects of ginger versus echinacea versus the combination of the two.
In the second study, a total of 154 patients (133 analyzed in per protocol collective) at least 12 years old with acute sore throat were given either an echinacea/sage spray or a chlorhexidine/ lidocaine spray with two puffs every 2 hours, in a double-dummy blinded manner, up to 10 times daily until they were symptom-free, for a maximum of 5 days (8).
The primary outcome of the study was defined as a decrease of at least 50% of the total symptoms compared to baseline. Secondary parameters were defined as time to becoming symptom free, throat pain, and global assessments of efficacy by the physician and patient.
There was no difference in either the primary or secondary outcomes between the two treatment arms of the study. This study was included here as it does relate in some way to pain but can hardly be taken as proof that echinacea is an analgesic.
Bottom line
There is no scientific proof that echinacea helps alleviate pain.
Does it Function as a Laxative?

Diarrhea is a documented side effect of echinacea but there are no studies, case reports or laboratory studies to directly support the role of echinacea as a laxative.
Bottom line
There is no science behind any claim that echinacea acts as a laxative.
Is it an Anti-inflammatory?
There are only five small clinical studies looking at the anti-inflammatory effects of echinacea. None of these studies addressed the big picture of inflammation.
One looked at echinacea as adjunctive therapy in carpal tunnel syndrome (9). There was a slightly better pain trend in the echinacea, ALA, quercetinquercetin, versus shock wave therapy in 60 men.
Three of the other studies looked at gingivitis and the last was a Russain study looking at echinacea as an immunomodulator in wounds (but no English version of the paper is available to comment on the quality of the study.)
Bottom line
There is essentially nothing to support echinacea as an anti-inflammatory.
Is it good for the skin?

Canadian investigators found a beneficial effect of echinacea in acne (in vitro) and attributed this to a combination of an antibacterial and anti-inflammtory effects (10).
A complex three part German/Hungarian study showed that echinacea can reduce inflammation related to atomic eczema (11).
The effect of echinacea formulations (gland cream) on skin irritation, hydration level and wrinkle reduction was evaluated in 10 healthy volunteers, aged 25-40 years (12). Echinacea purpurea cream and gel developed in this study were effective in improving skin hydration and reducing wrinkles, but showed low storage stability.
Another small study (in vitro) showed that echinacea may exert an anti-photageing effect (13).
Bottom line
My PhD supervisor would summarise all the above research by saying that ''there are some 'scrappy-do' studies looking at echinacea in skin health''. I am not sure that 'scrappy-do' is a real word but I know exactly what he means. There are random bits of unrelated low quality research but nothing of merit to suggest that echinacea has a role in dermatological conditions.
In the safety section, we will see that echinacea has been associated with some significant adverse skin reactions (and that gets a bit confusing as we will see).
Does It Improve Mental Health?
Just one small study looks at echinacea in mental health.
Hungarian investigators looked at both animals and healthy volunteers for this study (14). Echinacea reduced anxiety in rats who were tested on an elevated maze. In the human study, healthy volunteers scoring high on the State-Trait Anxiety Inventory (STAI) were given either 20 mg or 40 mg of echinaea plant extract for one week.
Data were collected using a structured self-assessment diary technique. The high dose (40mg) decreased STAI scores within 3 days in human subjects, an effect that remained stable for the duration of the treatment (7 days) and for the 2 weeks that followed treatment. However no benefit was noted in the 20mg group.
Bottom line
From a clinical perspective, this is an extremely small and very short term study making it impossible to infer anything meaningful about the mental health effects of echinacea.
Is It Good For Upper Respiratory Problems?

A collaboration from Austria, Germany and the USA prepared a full Cochrane review of echinacea in the prevention and treatment of the common cold (15).
The reviewers noted that echinacea plant preparations are widely used in Europe and North America for coughs and colds. In the introduction to the review, the authors point out that both consumers and physicians are unaware that products sold and marketed as echinacea cold remedies differ appreciably in their composition.
This variability is due to different plant parts, different extraction methods and the addition of other components according to the reviewers (which we have already noted).
The review focused on randomised controlled trials of mono-preparations of echinacea versus placebo.
A total of 24 trials involving 4631 study participants were included in the meta-analysis. Of these trials:
- 9 addressed prevention
- 14 addressed treatment and
- 1 addressed treatment and prevention.
Overall the prophylaxis studies showed a positive (but not statistically significant) trend while the treatment trials showed no benefit. The review found that echinacea might reduce the relative risk of catching cold by 15%. This means that if 500 out of 1000 people taking placebo caught a cold, then 425 people on echinacea would catch a cold.
Bottom line
Research shows a positive but non statistically significant positive trend in there use of echinacea for prevention of colds but no benefit in treatment.
Is Echinacea (and or Supplementation) Safe?
There are several safety concerns when it comes to echinacea.
Studies have shown that echinacea products vary greatly and that labelling of products may be incorrect . This may not be a safety issue directly related to echinacea itself but is certainly a safety concern for the end user.
Canadian investigators studied the content of 10 different commercial products of Echinacea angustifolia or Echinacea purpurea were selected (16).
They purchased 3 bottles of each from 2 different lots. The investigators were blinded to product identity before phytochemical analysis. Lot-to-lot variation was small, but product variation due to species and formulation was large.
Overall alcohol based tinctures had lower levels of polysaccharide and high levels of alkalised and were noted to have antiviral but limited immunomodulatory effects. Aqueous based products had higher levels of polysaccharides and lower levels of alkamides than the alcohol based products.
A second study of 50 products purchased in Denver, Colorado found that 10% contained no echinacea and 57% failed to meet the quality standards described on the label (17). Would this be a bad time to remind us all of the $15.1 million spent on echinacea? This Colorado study suggests that $1.5 million was spent on products that don't contain echinacea in one year alone. Oops.
Another key concern related to echinacea is allergy. Allergic reaction are the most common side effect of echinacea and are especially seen in patients who are allergic to ragweed (18).
Additionally one study found a 5% increase in rash in children who took echinacea (19).
Cases of the skin condition erythema nodosum have been reported and attributed to echinacea (20). (Please forgive me while I divert for a moment. Up To Date is the bible for doctors. Almost every clinic and hospital in the world provides access to Up To Date.
Well, Up To Date says that echinacea causes pemphigus vulgaris but actually uses a reference for erythema nodosum. I am pretty shocked as I assumed that Up To Date was the real deal. Apparently not. Don't worry I am about to email the editor of Up To Date to suggest an amendment but again it reminds me of the importance of doing my own research).
Back to the task at hand.
Other reported side effects of echinacea include dyspepsia, diarrhoea, fever, nausea and vomiting.
The German Drug Regulatory authority recommends that echinacea preparations should not be taken for longer than eight weeks due to a lack of longterm safety data.
Equally parenteral echinacea is not recommended due to lack of safety and efficacy data.
It is also recommended that echinacea be avoided during pregnancy and lactation despite the fact that a systematic review found no evidence of teratogenicity (21).
A single case of possible echinacea related anaphylaxis was reported in a lady with atopy (22). As she also took some other dietary supplements, it would be unfair to blame echinacea at this stage.
Despite the lack of compelling evidence to support echinacea as an immuno-modulator, it is generally recommended that echinacea be avoided in patients with autoimmune disorders because of a risk of exacerbation of any underlying autoimmune tendency.
A case of Sjogren’s syndrome related renal tubular acidosis has also been reported in the medical literature (23).
Echinacea is a modulator of cytochrome P350 3A4and cytochrome P4502A1. It inhibits intestinal P450 3A4 (which raises the possibility of toxic levels of co-administered drugs handled by the same system). It also induces hepatic cytochrome P450 3A4 (which can lower the levels of some drugs handled by the same system).
As a side note, nature is pretty amazing. The fact that echinacea inhibits one part of the drug metabolising system and induces another part is a very smart in-built homeostatic control mechanism.
Back to the task at hand again.
The take home message here is that there are multiple opportunities for drug-drug interactions and the net effect of induction-inhibitor makes it difficult to predict the net effect on any co-administered drug.
Not only is echinacea one of the top selling herbs products worldwide it is also one of the top selling herbs among people with HIV infection.
Many anti-HIV drugs are metabolised by the cytochrome P450 enzyme system. Maintaining anti-HIV drug levels above the minimum inhibitory concentration of the virus is mission critical to prevent the emergence of uncontrolled or viral resistant strains (24).
https://www.ncbi.nlm.nih.gov/pubmed/21078942
The authors concluded that monitoring darunavir concentrations may be necessary to avoid the mergence of viral blips.
Echinacea does contain pyrrolizidine alkaoids which are known to be hepatotoxic. However, the pyrrolizidine alkaloids in echinacea do not contain the 1,2 saturated ring which specifically causes hepatotixicity.
Conclusion
The current state of research on echinacea is utterly frustrating. It is really just a good example of the Swiss cheese model (where errors at multiple levels expose individuals to risk).
Let's take these errors one by one:
- Researchers have failed to live up to ICH-GCP standards which mandate that all human clinical research is meaningful and contributes to our overall knowledge base. Despite plenty of studies on echinacea, we know very little at the end of the day. Going forward, all research on echinacea should use standardised products.
- Manufacturers are producing poor quality and mislabelled products. Essentially people who buy echinacea are buying the equivalent of a lucky bag. The content can vary wildly from band to brand and between lots. This likely explains that huge variability in results that are seen in the clinical trials and in individual experience of using echinacea.
- Bloggers and 'e-pseudoexperts' have (again) inflated and misrepresented the results of the poor quality studies that we have.
- Even Up To Date has made errors on echinacea
All in all, when it comes to echinacea, let's just say buyer beware.
Meanwhile, I am off to email Up To Date to get that error fixed.
Addendum: Special shout-out to Up To Date who responded instantly to my email, reviewed my observation, amended the entry on their site and even sent me a nice thank -you email. Very professional and re-assuring indeed.

Leave a Reply