L-methionine (L-Met), aka methionine, is an amino acid needed to form protein in the body. It also has, as I have discovered, many other valuable claims attributed to it.
What are some of those claims?
These are some of the ones I’ve come across and will be tackling: assists with drug withdrawal symptoms, lessens tremors associated with Parkinson’s disease, reduces the risk of colorectal cancer, builds bone strength, and is useful as an aid in weight loss.
What Is L-Methionine?
J.H. Muller, a researcher at Columbia University in New York, first discovered methionine in 1922 when he isolated a “sulfurous amino acid.” However, as the story goes, he submitted an incorrect formula. Three years later, his colleague in Japan would correct the formula and named it “methionine.” Six years later, G. Barger and F.P. Coyne defined its structure.
These findings were followed up during the post-war years, to treat the chronic protein insufficiency suffered by soldiers returning home from the war. In 1946/47, the first technically feasible synthesis of L-Met was achieved (1).
L-Met is one of nine essential amino acids, and it is important for many body functions, including growth and tissue repair (2). Amino acids, themselves, are the building blocks of protein. Those that are termed “essential” cannot be made by the body and so, must come from food.
This is because they have carbon skeletons that cannot be made from simpler molecules, to meet the body’s needs. What foods supply L-Met? As it goes on to form protein, food sources of protein – such as legumes, nuts, meat, fish, and dairy – are dietary sources of the amino acid (2).
Structurally, L-Met is a sulfur-containing L-amino acid with molecular formula C5H11NO2S. It is needed to make the amino acid cysteine, being the accepted metabolic precursor. Only the sulfur atom from L-Met is transferred to cysteine; the carbon skeleton of cysteine is donated by serine. Aside from L-Met, cysteine is the only other sulfur-containing amino acid (2, 12).
Is There Any Research?
A PubMed search for papers with the search terms “L-methionine” or “methionine” included in the title, in the English language, returns just over ten thousand papers. Narrowing that down to human-specific papers only, the terms offer a little less than three thousand papers. Of these, how many are high-quality meta-analyses or systematic reviews? Forty – spanning from 1994 to the current year, 2017.
How does this summary of the research into L-Met compare to the research on something else popular? Amino acids, including L-Met, are the building blocks of protein. There are many protein supplements on the market. A search for quality papers (meta-analyses or systematic reviews) on protein returned over a thousand papers, and that’s for papers specific to humans alone.
Let’s address some of the specific claims, individually. Again, I focus on powerful meta-analyses and systematic reviews, which provide the best-quality evidence available, relevant to humans and in the English language.
Does L-Methionine Reduce the Risk of Colorectal Cancer?
L-Met has been implicated in colorectal cancer risk. There are, however, inconsistencies within the literature, with some studies showing restriction of L-Met to have tumor-inhibitory effects, whereas others suggest excess to have adverse outcomes (4, 5).
I found one meta-analysis addressing dietary L-Met intake in this context, from 2013. It looks at 8 prospective studies involving 431,029 participants with 6,331 colorectal cancer cases identified. Their findings indicate that dietary L-Met may be associated with a decreased risk of colorectal cancer, especially colon cancer. However, they acknowledge that more prospective studies with longer follow-up time were needed to confirm these findings (4).
There is one systematic review in an animal (mouse) model. It looks at the role of L-Met and folate in intestinal tumor development. It found that nutritional modulation of L-Met had different effects on intestinal cancer dependent on such things as dosage, and duration and timing of the intervention (5).
Bottom Line
Minimal quality evidence, specific to humans, of a role for L-Met in reducing the risk of colorectal cancer. Better-quality research is needed to be conclusive.
Does It Lower Tremors in Patients With Parkinson’s?
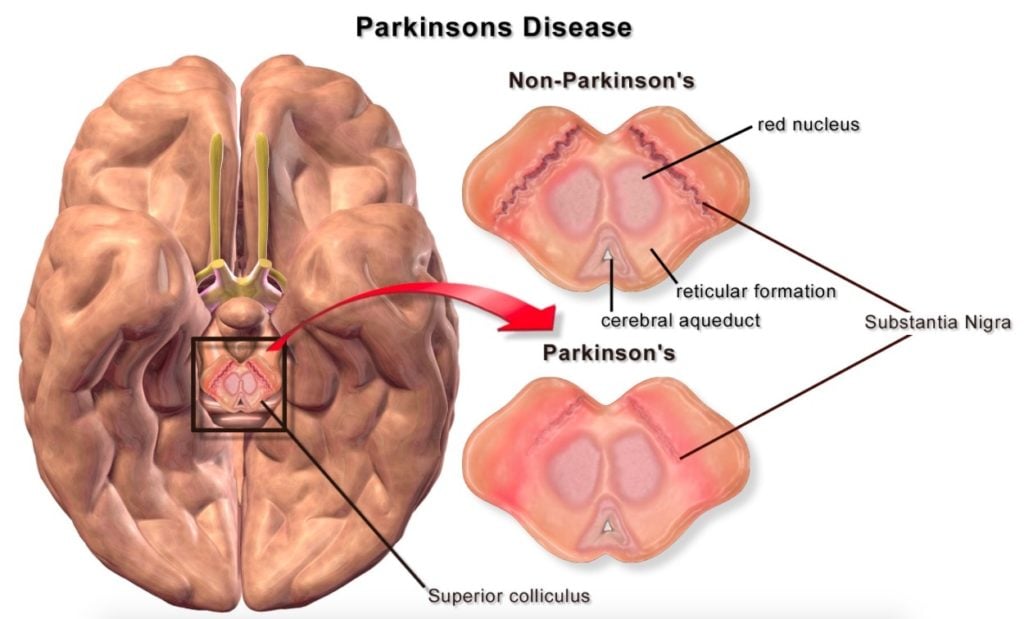
I was unable to find any papers, let alone meta-analyses or systematic reviews, of a role for either L-Met or SAMe (S-adenosyl-L-methionine) in Parkinson’s disease. I extended the search to include both human and animal studies.
Bottom Line
No quality evidence of a role for L-Met in reducing tremors in patients with Parkinson’s disease.
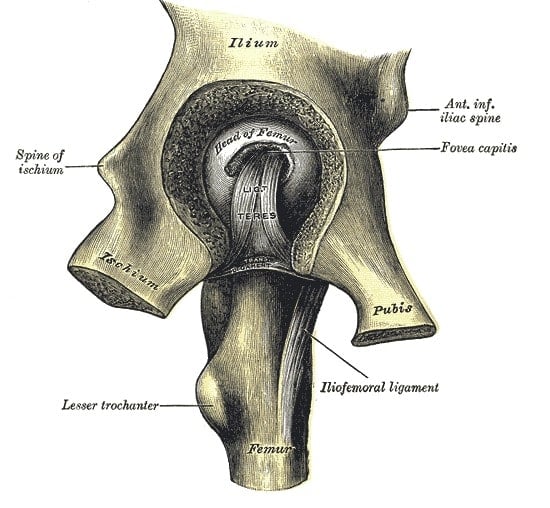
Does It Build Bone Strength?
No quality papers were available that support a role for either L-Met or SAMe in building bone strength, in human or animal studies, according to my search.
We can compare this to the evidence available for Cissus Quadrangularis (CQ), a traditional Ayurvedic medicinal plant, which we’ve explored previously. A 2017 meta-analysis, assessing the overall efficacy and safety of this plant, included three studies of patients with bone fractures. The results were positive for a role in bone fracture healing and bone pain reduction, with CQ shown to influence bone in a number of ways.
Bottom Line
No quality evidence of a role for either L-Met or SAMe in building bone strength.
Does It Aid Weight Loss?
I was unable to locate neither meta-analyses nor systematic reviews of a role for either L-Met or SAMe in weight loss. I extended the search to include animal studies and, likewise, was unable to find any quality evidence here.
Bottom Line
No available quality evidence suggesting a role for L-Met, or SAMe, in assisting with human weight loss.

Does It Help People Dealing With Drug Withdrawal?
Neither systematic reviews nor meta-analyses were found in this category. The search terms included L-Met and SAMe, drug withdrawal, detox, and detoxification.
Bottom Line
No quality evidence suggesting a role for either L-Met, or SAMe, in drug withdrawal support in humans.
Does It Support Good Liver Function?
I could not find any papers for L-Met, specifically, in the context of improving liver function. It is noted, in a reputable online source (PubChem), that L-Met “helps to lower cholesterol levels by increasing the liver’s production of lecithin, and reduces liver fat. It may also protect against the toxic effects of liver toxins, such as acetaminophen.” (2)
How it achieves this is not entirely clear. It is thought that the metabolism of high doses of acetaminophen in the liver leads to decreased levels of liver glutathione, an antioxidant, and increased oxidative stress. L-Met is a precursor to L-cysteine, which may have antioxidant activity.
L-cysteine is also a precursor to the antioxidant glutathione. Antioxidant activity of L-Met and metabolites of L-Met appear to account for its possible liver-protective activity. Recent research suggests that L-Met itself has free-radical-scavenging activity by virtue of its sulfur, as well as its chelating ability (6).
There are a few systematic reviews and meta-analysis papers looking at SAMe’s effects on liver disease. SAMe is the main methyl donor in methyl-transferase reactions, and it is well established that SAMe supplementation restores liver glutathione levels, the main cellular antioxidant, and reduces the effect of liver injury.
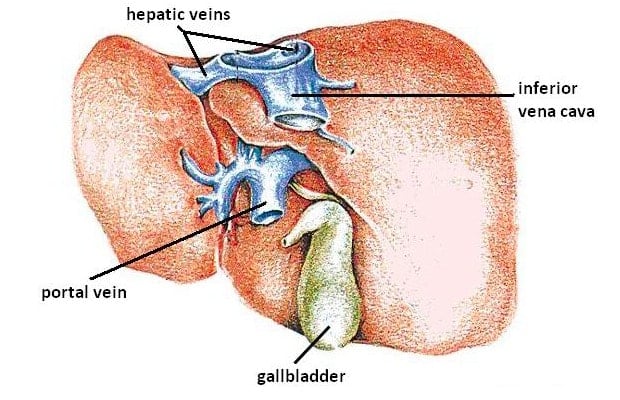
SAMe levels within liver cells can influence diverse pathophysiological processes, including tissue oxidative state, liver cell death, and malignant transformation. Its synthesis is lowered in chronic liver disease. Pre-clinical studies indicate this could worsen liver injury, and SAMe supplementation may be useful. It’s been widely used in Eastern Europe, Russia, China, Southern Asia, and South America for chronic liver disease. (7)
A fairly recent (2015) systematic review and meta-analysis (8) looked at SAMe for the treatment of chronic liver disease. Their findings suggest that SAMe could be used as the basis of a medication regimen for liver function improvement because of its safety. However, SAMe also demonstrated limited clinical value in the treatment of certain chronic liver diseases.
A 2012 paper reviewed the role of SAMe in liver disease (7). As no large, high-quality, randomized trials had been performed that definitively establish clinical usefulness in specific disease states, they were unable to conclude a role for SAMe in liver function.
Interestingly, caution has been advised in the use of L-Met in patients with severe liver damage, as it may aggravate liver encephalopathy (the loss of brain function when a damaged liver doesn’t remove toxins from the blood) (9).
Bottom Line
Some evidence and quality literature is available of a role for L-Met, and weak evidence of a role for SAMe, in supporting liver function in humans. Larger, better-quality trials are needed to be conclusive. Caution is advised in those with existing, severe liver damage.
Does L-Met Have Any Proven Benefits?
According to PubChem, there are benefits derived from L-Met, largely due to its sulfur content. PubChem is a database of chemical molecules and their activities against biological assays. The system is maintained by the National Center for Biotechnology Information (NCBI), a component of the National Library of Medicine, which is part of the United States National Institutes of Health (NIH).
For instance, due to the inclusion of sulfur, “L-Met improves the tone and pliability of skin, hair, and strengthens nails. Valuable in many detoxifying processes, the sulfur provided by L-Met also protects cells from pollutants, slows cell aging, and is essential for the absorption and bio-availability of selenium and zinc.
L-Met chelates heavy metals, such as lead and mercury, aiding their excretion. It also acts as a lipotropic agent and prevents excess fat build-up in the liver.” (2) L-Met and cysteine are, uniquely, the only sulfur-containing amino acids – the latter of which derives its sulfur from L-Met.
The sulfur from L-Met can also be used to form a valuable compound known as S-adenosyl-L-methionine (SAMe), which has known anti-inflammatory activity (3).
Is L-Met Safe & Are There Interactions?
L-Met may cause nausea, vomiting, drowsiness, and irritability. It should not be used in patients with acidosis. It may aggravate hepatic encephalopathy (the loss of brain function when a damaged liver doesn’t remove toxins from the blood) in patients with established liver damage, so it should be used with caution in patients with severe liver disease (9).
L-Met is known to exacerbate psychopathological symptoms in schizophrenic patients, though there is no evidence of similar effects in healthy subjects.
The role of L-Met as a precursor of homocysteine is the most concerning aspect. Elevated homocysteine has been used as an indicator of the susceptibility to cardiovascular disease. A “loading ” of methionine (0.1 g/kg) has resulted in a short-term increase in plasma homocysteine levels. Although this procedure results in vascular dysfunction, it is short-term and unlikely to result in permanent damage. However, a tenfold larger dose, given mistakenly, resulted in death.
In a study of the possible relationship between homocysteine and Alzheimer’s disease, the death of a control subject after an oral load of L-Met, is reported (10). The subject developed post-load plasma concentrations of L-Met far beyond those reported previously in humans given the usual oral loading dose of L-Met (100 mg/kg body weight). The most likely explanation is that the subject received an overdose of the amino acid.
Longer-term studies in adults have indicated no adverse consequences of moderate fluctuations in dietary L-Met intake, but intakes higher than 5 times the normal dose resulted in elevated homocysteine levels. These effects of L-Met on homocysteine and vascular function are moderated by supplements of vitamins B6, B12, C, and folic acid.
In infants, L-Met intakes of 2 to 5 times normal resulted in impaired growth and extremely high plasma L-Met levels, but no adverse long-term consequences were observed (11).
Conclusion
Based on the currently available, quality evidence for L-Met, and specifically relating to the claims listed above that have been made for this essential amino acid, there is really not much to go on. There are about forty powerful papers, but very few of them specifically address the claims made above.
Dietary intake of the amino acid seems to be sufficient, and excessive doses of L-Met may be a cause for concern. It is an “essential” amino acid, but clearly not so “essential” with regards to some of its currently circulating claims.

Leave a Reply