Living in today's fast-paced society can mean our bowel motions slow down to a halt.
Literally.
We all know the effects of travel, stress and poor eating habits…. Constipation!
Constipation, infrequent bowel movements or difficulty in passing stools, is a common and uncomfortable complaint. It is suspected to affect upwards of 15% of all Americans according to the American Society of Colon and Rectal Surgeons [1].
The causes of constipation include a lack of fiber in diet, sedentary lifestyle, dehydration, aging, medication or a medical condition.
Generally, constipation is prevented by following the three basic steps to good gut health: a healthy diet, good water intake, and physical activity, and is fairly easy to treat if and when it occurs.
Although these lifestyle changes prevent or relieve constipation, for some people, a laxative may occasionally be required. Many safe, effective over-the-counter laxatives are available to treat occasional constipation.
Laxatives work in different ways, and the effectiveness of each laxative type varies from person to person. However, it's very important to read the label directions carefully and to only use them as directed as overuse of laxatives may cause serious side effects.
As more and more people are looking for healthier lifestyles, there is a growing interest in natural alternatives to chemical laxatives. But do they really work? Read on for an in-depth look at the research….
Table of Contents
An Uncomfortable Topic: Constipation
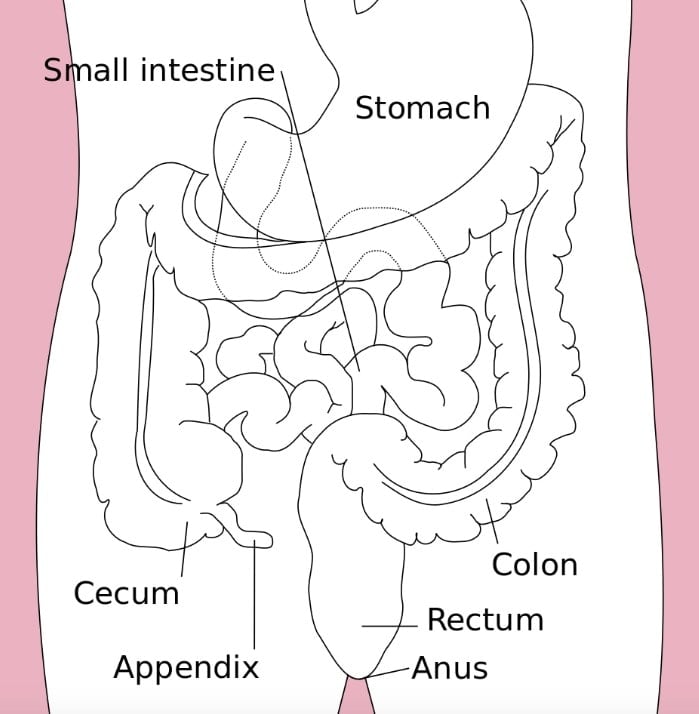
So what is normal bowel function? After eating, food moves through the small intestine, where it is broken down and the nutrients are absorbed. The remaining liquid waste then passes into the colon, where water and certain electrolytes are removed, turning the liquid waste into a more solid form. This product, known as stool, or poop, then passes into the rectum, where it is stored until bowel movement time.
The following three steps are known to prevent or ease constipation:
- Fiber
Eating a diet rich in fiber (whole-grain bread, nuts, fresh fruits, and vegetables). Unfortunately, most Americans don't eat enough dietary fiber.
The Institute of Medicine, which provides evidence-based advice on medicine and health, advises that adults should have around 25g of fiber per day for women and 38g per day for men. The recommended amount drops slightly for adults aged over 50 [2].
But not all fiber is the same! There are two types of fiber, soluble (which dissolves in water and may form a gel) and insoluble (which does not dissolve in water). Almost all plants contain both soluble and insoluble fiber.
Soluble fiber can help to lower cholesterol and regulate blood glucose (sugar) levels. Examples of soluble fiber include oats, many fruits and vegetables, beans, barley, and psyllium.
Insoluble fiber adds bulk to the stool and thereby contributes to bowel regularity. Examples of insoluble fiber are whole-wheat flour, wheat bran, and some vegetables.
- Water
Fiber works best when it absorbs water, making your stool soft and bulky, says the Mayo Clinic [3]. Drinking six to eight glasses of water per day also helps keep the stool moist, which makes it easier to pass.
- Exercise
Lastly, regular exercise, which can be as simple as taking a brisk walk for 30 minutes per day, is recommended to improve bowel movements.
How Do Laxatives Work On Bowel Function?
Laxatives work by containing chemicals that help increase stool motility (how fast it moves through the bowel), stool bulk (volume) and stool moisture. The main types of laxatives are bulk formers, osmotic, stimulant, and softeners. Different laxatives have different side effects too.
Bulk formers absorb water to form soft, bulky stool, prompting normal contraction of intestinal muscles. Bran and psyllium are the most common bulking agents. Some people are allergic to psyllium and therefore should not take it.
Osmotic laxatives are medications that draw water into the stool, resulting in softer stools and more frequent, easier to pass bowel movements. Some commonly used osmotic laxatives include polyethylene glycol (PEG), milk of magnesia, and lactulose.
Stimulant laxatives induce bowel movements by increasing the contraction of muscles in the intestines. Examples of stimulant laxatives include aloe, cascara, senna compounds, bisacodyl, and castor oil.
Stool softeners add moisture to the stool to allow easier bowel movements. Docusate sodium and docusate calcium are commonly used as stool softeners or emollient laxatives. These act by increasing the penetration of fluid into the stool, thereby softening it.
How Well Researched Are Laxatives?
Laxatives are the most commonly prescribed pharmacological interventions, so a good evidence base is important, and prescribing of bulk-forming laxatives is decreasing yearly, while that of stimulant and osmotic laxatives is increasing [4].
There is a good body of research to show that laxatives are quite safe when used cautiously, intermittently when possible, and in the absence of contraindications [5].
How Effective Are Laxatives? What Does The Research Say?
Large analyses of the pooled results of research studies have been conducted to determine the safety and efficacy of laxatives.
Research in Adults
One of the main reviews of laxative effectiveness in adults, which was conducted by Petticrew et al., analyzed all the research on the effectiveness of the four main types of laxatives used in the treatment of constipation in adults [6].
This study analyzed the results of two systematic reviews and 21 other studies on the effectiveness of laxatives in adults.
This review concluded that bulk former (fiber-based) laxatives (bran and psyllium are the most common bulking agents) and osmotic laxatives (including lactulose and PEG) were associated with increases in frequency and improvements in stool consistency and symptoms of constipation… ie they were effective. However, the researchers concluded that there was little evidence available as to the comparative effectiveness of bulk and non-bulk laxatives.
The results showed that bulk laxatives were associated with an increase in the frequency of 1–2 bowel movements per week compared with placebo and may be better tolerated than other laxative products.
Researchers stated that more research should be conducted into the effectiveness of overall dietary change (including increased fluid intake) in the treatment of constipation. They also noted that there “is a pressing need for large comparative trials of different strategies for the management of constipation in adults…which include comparisons of the effectiveness of different classes of laxative”.
Research in Children
One of the best reviews of laxative use in children is a recent Cochrane review published in 2016 by Gordon et al. The study thoroughly analyzed the medical literature on laxatives used in children to date [7]. The researchers studied whether osmotic and stimulant laxatives were effective in the treatment of childhood constipation and whether these medications cause any adverse effects.
This review included 25 studies with a total of 2310 children (with participants aged 0 to 18 years old) and compared ten different laxative agents to either placebo or each other. Many of the studies were small in size and were judged to be of poor or unclear quality. Only thorough, randomized controlled trials (RCTs), which compared osmotic or stimulant laxatives to placebo or another intervention were considered for inclusion.
The results of the review suggest that PEG preparations may increase the frequency of bowel movements in constipated children (ie they worked), with only minor side effects that were generally lower when compared to other agents. Common side effects included flatulence, abdominal pain, nausea, diarrhea, and headache. There was also evidence that liquid paraffin (mineral oil) increased the frequency of bowel movements in constipated children (ie it worked). Common side effects included abdominal pain, distention, and watery stools.
The study authors recommended that the results of the pooled analyses should be interpreted with caution because of quality and methodological concerns, and expressed concern at the lack of long-term studies on laxative use, which is particularly relevant given that the nature of constipation in children is chronic.
Are Over The Counter Laxatives Dangerous?

Well…. Yes and no.
Many safe, effective over-the-counter laxatives are very helpful for treating occasional constipation, provided they are used with caution. It's very important to read the label directions carefully and to only use them as directed as overuse of laxatives may cause serious side effects.
According to the review by Petticrew et al., few studies used standardized outcome measures to assess adverse effects, although most studies did not report an increase in pain with fiber or non-bulk laxatives. Two of the trials examined improvements in general wellbeing, neither of which showed any difference between fiber and other laxatives.
The review by Gordon et al. demonstrated that no serious adverse events were reported. Adverse events included flatulence, abdominal pain, nausea, diarrhea, and headache. But guess what? The common adverse events in the placebo-controlled studies included flatulence, abdominal pain, nausea, diarrhea, and headache. So there was not much difference in adverse effects that could be attributed to the laxatives anyway.
Overall the research shows that laxatives are quite safe when used cautiously, intermittently when possible, and in the absence of contraindications.
What are the Risks of Laxatives?
Laxatives can interfere with your body's absorption of certain medications and nutrients. They can interact with some antibiotics, and certain heart and bone medications.
Laxatives can have serious side effects, especially after prolonged use. They can decrease your colon's ability to contract and actually worsen constipation.
These side effects include dehydration and abnormal levels of electrolytes (this includes calcium, chloride, potassium, magnesium, and sodium) in the blood, which can lead to serious complications, such as kidney damage, abnormal heart rhythms, weakness, confusion, seizures and even death [8].
In general, bulk-forming laxatives also referred to as fiber supplements, are the gentlest on your body and safest to use long term. Bulk-forming laxatives and stool softeners are generally safe to use during pregnancy, but stimulant laxatives may be harmful.
In recent reviews of harmful side effects reported by consumers and health care professionals over the past few years, the FDA has identified 54 cases of serious side effects associated with the use of over the counter laxative products containing sodium phosphate [9]. Thirteen cases were fatal, including one child and 12 adults.
According to the FDA, “the label of sodium phosphate laxatives states that they should be used as a single dose taken once a day, and the products should not be used for more than three days. Equally important, consumers who do not have a bowel movement after taking an oral or rectal dose should not take another dose of the product. In addition, labeling instructs adults and children to ask health care professionals before using these products if they have kidney disease, heart problems or dehydration9.”
FDA is now warning that adults older than 55 and adults and children with certain health conditions should ask a health care professional before using these products because they may be at increased risk for harmful side effects. Laxative products containing sodium phosphates are marketed under the brand name "Fleet" and may also be present in-store brand and generic products9.
What Are Natural Laxatives?
“Natural Laxatives” are foods that help the gut with digestion and regular bowel movements. Some people prefer to use natural options to laxatives where possible, for a variety of reasons, including knowing what they are putting in their body, cost, and avoidance of any adverse effects or risks. This has led to an interest in these so-called natural laxatives.
How Well Researched Are Natural Laxatives?
Let’s have a look at the most discussed natural laxatives:
Aloe Vera
Aloe vera is a plant that contains anthraquinone derivatives, which are known to have a stimulant effect. Aloe vera has therefore been traditionally and commonly used as a treatment of constipation.
Evidence exists on anthraquinone glycosides having a laxative effect, in fact, so much so that aloe vera laxative preparations have been approved by the German Commission Governmental regulatory agency for use in the treatment of constipation as a second-line agent.
A review of the evidence on the laxative effect of aloe vera was published in 2008
Aloe vera latex is commonly used in the treatment of constipation (de Witte 1993); the laxative effect of the anthraquinone glycosides found in Aloe vera latex is well established (Ulbricht et al. 2008).
In subjects with chronic constipation, a novel preparation containing Aloe vera, celandine, and psyllium was found to improve a range of constipation indicators (bowel movement frequency, consistency of stools, and laxative dependence) in a 28-day double-blind trial; however, the effect of Aloe vera alone was not investigated in this study (Odes and Madar 1991).
However, aloe vera is not recognized as an over-the-counter laxative by the U.S. Food and Drug Administration due to a lack of sufficient data to establish its safety and efficacy for use as a laxative [10].
In summary, more research needs to be done before it can be recommended as a safe and effective laxative.
Chia Seeds

Chia seeds are a quick and easy source of protein, healthy fats, dietary fiber, minerals, vitamins, and antioxidants [11]. With 10 grams per ounce, they are an excellent source of according to the Academy of Nutrition and Dietetics Academy. Chia seed contains between 34 and 40 g of dietary fiber per 100 g, equivalent to 100% of the daily recommendations for the adult population!
No specific evidence exists on the effect of chia seeds as laxatives, although their impressive fiber content alone would assist with constipation. Research to assess the effectiveness of chia seeds compared to chemical laxatives has not been done.
Flax seeds
Very limited evidence exists to suggest that flaxseed oil and mucilage shows laxative activity. Though interesting, research has not been published in humans, only in animals. As a good source of fiber though, flaxseed (not flaxseed oil) would have some effectiveness as a laxative.
It is important to note that in large doses, or when taken without enough water, flaxseed may cause bowel obstruction [12].
Green leafy vegetables

Leafy greens are another excellent source of fiber. Although leafy vegetables are great for bowel health and regularity, no specific evidence exists on their role as laxatives neither as a comparison to chemical laxatives.
High fiber fruit
As with leafy greens, high fiber fruits are another excellent source of fiber, but, no specific evidence exists on their effectiveness as laxatives, nor a comparison to chemical laxatives.
It has been proposed that fruit may assist gut health by increasing bulk and liquid in the diet and/or by fermentation in the colon. Fruits contain mostly sugars and fibers, such as pectin, that are extensively fermented in the large intestine. Certain fruits, especially apples and pears, are concentrated in fructose, which is poorly absorbed and has been suggested to function similar to dietary fiber, escaping absorption in the small intestine while being fermented in the large intestine [13]. Accordingly, apple and pear juices are often used to treat constipation in children.
Coconut Water

Though many people do find coconut water to have a laxative effect, no research exists to confirm this.
Probiotic foods
Probiotics create a healthy environment in the gut microflora (bacteria) to keep the digestive system free of issues like constipation and diarrhea. Probiotic foods include sauerkraut, kimchi, and probiotic yogurt. A 2014 study found that on average, probiotics slowed “gut transit time” by 12.4 hours but increased the number of weekly bowel movements by 1.3, and helped soften stools and make them easier to pass [14].
This and other studies are showing more and more evidence that probiotics assist proper bowel health and can act as laxatives. However, there is currently not enough evidence to compare probiotics to chemical laxatives.
Other Possible Laxatives
Some people have asked about the effectiveness of fruits as laxatives, such as grapes, figs, raisins, apples, cherries, prunes, dates, pears, avocados, nectarines, and blueberries. Again, these all have good amounts of fiber and water and are therefore great for healthy bowel function.
For these reasons, they may act as laxatives (for some people, and especially in high quantities). But the research does not currently demonstrate a conclusive laxative effect that is comparable to chemical laxatives.
Conclusion
The research shows that laxatives are quite safe when used cautiously, intermittently when possible, and in the absence of contraindications.
Although some people prefer to use natural options for laxatives where possible, there just isn’t enough conclusive, high-quality evidence in place to support their effectiveness, nor to show that these are as effective as chemical laxatives.
In this case, as often happens, “natural” doesn’t necessarily mean “better”.
More research is needed to study the long-term use of laxatives, and the efficacy of some of the promising natural laxatives mentioned above, such as aloe vera and probiotics….

Leave a Reply