Intro
If you’re tossing and turning in bed, you might be tempted to brew some Sleepytime® or similar herbal tea to drink. If so, you’ve probably already tried valerian root. It has been used since ancient times as a sleep aid as well as for reducing anxiety and stress. It’s also been used for neuralgia, shell shock, epilepsy and to relieve digestive and other spasms of smooth muscles.
But is there any scientific evidence that supports its use in any of these or other conditions? I’ve reviewed the current scientific literature to put these claims to the test.
What Is Valerian Root?
Valerian root (valeriana officinalis) is a perennial flowering plant, with heads of sweetly scented pink or white flowers that bloom in the summer and can reach a height of 5 ft. It is native to Europe and Asia but now grows in most parts of the world. The name is derived from the personal name Valeria and the Latin verb valere (“to be strong, healthy”). Other names include setwall (English), Valerianae radix (Latin), Baldrianwurzel (German), and phu (Greek). The genus Valerian includes over 250 species, but V. officinalis is the species most often used in the United States and Europe.
Valerian has been used as a medicinal herb since at least the time of ancient Greece and Rome. Hippocrates described its properties, and Galen later prescribed it as a remedy for insomnia. In medieval Sweden, it was sometimes placed in the wedding clothes of the groom to ward off the "envy" of the elves.[1]
The seventeenth century astrological botanist Nicholas Culpeper thought the plant was "under the influence of Mercury, and therefore hath a warming faculty." He recommended both herb and root, and said that:
"the root boiled with liquorice, raisons and aniseed is good for those troubled with cough. Also, it is of special value against the plague, the decoction thereof being drunk and the root smelled. The green herb being bruised and applied to the head taketh away pain and pricking thereof."[2]
According to the Principles and Practice of Phytotherapy[3] the root and rhizome of the valerian plant contain the biologically active ingredients and include:
- Iridoids: known as valepotriates (valeriana epoxy-triesters) including valtrate, isovaltrate, didrovaltrate and acevaltrate.
- Essential Oils: contains monoterpenes (mainly borneol, bornyl acetate), sesquiterpenes (beta-bisabolene, valernal (fresh root)) and carboxylic compounds (esters of valerianic/isovaleric acid).
- Non-volatile cyclopentane sesquiterpenes known as valerenic acid and its derivatives, flavonoids, amino acids, lignans, and low levels of GABA (gamma-aminobutyric acid- more about this later).
Preparations of valerian marketed as dietary supplements are made from its roots, rhizomes (underground stems), and stolons (horizontal stems). Dried roots are prepared as teas or tinctures, and dried plant materials and extracts are put into capsules or incorporated into tablets.
There is no scientific agreement as to the active constituents of valerian, and its activity may result from interactions among multiple constituents rather than any one compound or class of compounds. The content of volatile oils, including valerenic acids; the less volatile sesquiterpenes; or the valepotriates (esters of short-chain fatty acids) are sometimes used to standardize valerian extracts. As with most herbal preparations, many other compounds are also present.
In the United States, valerian is sold as a dietary supplement, and dietary supplements are regulated as foods, not drugs. Therefore, pre-market evaluation and approval by the Food and Drug Administration are not required unless claims are made for specific disease prevention or treatment. Because dietary supplements are not always tested for manufacturing consistency, the composition may vary considerably between manufacturing lots.
Valerian root is approved by the European Medicines Agency for the relief of mild nervous tension and sleep disorders. It has gotten this recommendation based on its “long-standing use”. (To understand what that means, see an explanation here.)

Is There Any Research?
As of February 2018, the biomedical literature (PubMed.gov) contained 232 articles about valerian root dating back to 1951. Most of these research studies involve experiments with laboratory animals (mostly rats and mice) or “test tubes” (in vitro studies). Of all the articles mentioning valerian root only 18 studies appear to involve human subjects.
Turning to the U.S. government’s database of clinical research trials (ClinicalTrials.gov), “valerian root” yields 11 studies. These studies involve the following medical topics: sleep, sedation, ADHD, anxiety, depression.
To put these findings in perspective, I searched for Temazepam (Restoril™) a prescription medication used for sleep disturbances. In PubMed there are 1062 studies of which 261 involve human subjects. There are 6 completed clinical trials in clinicaltrials.gov.
Does Valerian Root Help with Sleep?

Many chemical constituents of valerian have been identified, but it is not known which may be responsible for its sleep-promoting effects in animals and in vitro studies. It is likely that there is no single active compound and that valerian’s effects result from multiple constituents acting independently or synergistically.[4]
According to the Office of Dietary Supplements at the U.S. National Institutes of Health, two categories of constituents have been proposed as the major source of valerian’s sedative effects. The first category comprises the major constituents of its volatile oil including valerenic acid and its derivatives, which have demonstrated sedative properties in animal studies.
However, valerian extracts with very little of these components also have sedative properties, making it probable that other components are responsible for these effects or that multiple constituents contribute to them.[5] The second category comprises the iridoids, which include the valepotriates. Valepotriates and their derivatives are active as sedatives in vivo but are unstable and break down during storage or when dissolved in water, making their activity difficult to assess.
A possible mechanism by which a valerian extract may cause sedation is by increasing the amount of gamma aminobutyric acid (GABA) available in the brain. GABA is a key neurotransmitter (chemical messenger) that is widely distributed in the brain. GABA’s natural function is to reduce the activity of the neurons to which it binds.
The receptors for GABA in brain cells (neurons) are called channel receptors because, when GABA binds to them, they change shape slightly allowing ions to pass through their central channel. The channel mainly allows negatively charged chloride ions to enter the neuron, thus reducing its excitability.
Because of this property of the GABA channel receptor, GABA is classified as an inhibitory neurotransmitter, as opposed to excitatory neurotransmitters, such as glutamate, which augment the nerve impulses in the neuron. GABA is the natural “key” to “unlock” the GABA receptor’s channel. But GABA is not the only molecule that can modify this channel receptor’s opening. Other molecules can also affect it, such as the benzodiazepine medications used to treat anxiety.
In vitro studies published in 1994 suggested that that a valerian extract may cause GABA to be released from brain nerve endings and then block GABA from being taken back into nerve cells.[6] In addition, valerenic acid inhibits an enzyme that destroys GABA. Valerian extracts contain GABA in quantities sufficient to cause a sedative effect, but whether GABA can cross the blood-brain barrier to contribute to valerian’s sedative effects is not known.
What have studies with human subjects shown? In the classic studies on sleep and valerian by Leathwood and Chauffard[7, 8] in the 1980’s, 128 volunteers were given a valerian extract, extracts of valerian with hops, or a placebo for three nights. The researchers found that, subjectively, valerian shortened sleep latency (the time it takes to go from awake to sleep), and improved sleep quality compared to those who took the placebo. This was most pronounced in those who considered themselves poor or irregular sleepers.
However, three more recent reviews of the scientific literature questioned the effectiveness of valerian in the treatment of sleep disorders. In 2000, Stevinson et al[9] found 370 articles on the topic, but only 9 met their inclusion criteria of being randomized, placebo-controlled studies. They concluded that the findings were contradictory and there was great inconsistencies between the trials in terms of the patients used, the experimental designs and procedures, and the methodological quality that the results were deemed inconclusive.
A study by Taibi, Landis, Petry and Vitiello[10] in 2007 undertook a systematic review to examine the evidence on the efficacy of valerian as a sleep aid with specific attention to the type of preparations tested and the characteristics of the subjects studied.
“Most studies found no significant differences between valerian and placebo either in healthy individuals or in persons with general sleep disturbances or insomnia. None of the most recent studies, which were also the most methodologically rigorous, found significant effects of valerian on sleep.”
The last review in 2010 by Fernandez-San-Martin et al[11] suggested by valerian might be effective for a subjective improvement for insomnia, however its effectiveness was not demonstrated by any quantitative or objective measurements.
Bottom line
Although valerian root has been used as a sleep aid for millennia, scientific proof of its efficacy is currently inconclusive. More well-controlled studies with objectively measurable outcomes are necessary to prove or disprove valerian’s value as a sleep aid.
Does It Calm Anxiety?

Just as in sleep disorders, the role of GABA is an important one in the cause and treatment of anxiety disorders. Valerian has been studied for its effect on anxiety at multiple levels- in vitro, in vivo, and in clinical trials. These have been recently reviewed (January 2018) by Savage et. al[12].
In vitro studies: In vitro studies of valerian have concentrated on the sesquiterpene valerenic acid. Studies on brain tissue from male Sprague-Dawley rats [13], female Swiss-Webster mice [14] and male Wistar rats [6] indicate that valerian can modulate the GABA system by both increasing GABA release and by inhibiting the reuptake or degradation of GABA. Additional studies in rats and frogs found that valerenic acid acts at a specific site on GABA receptors. [15-17]
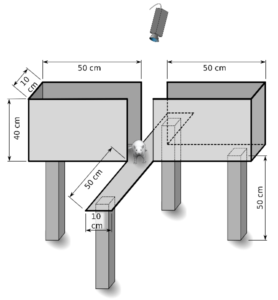 In vivo animal studies: Murphy et al[18] looked at anxiety in rats using an elevated plus maze (EPM). EPM is the most commonly employed animal behavioral model of anxiety. The test uses an elevated, plus-shaped (+) apparatus with two open and two enclosed arms.
In vivo animal studies: Murphy et al[18] looked at anxiety in rats using an elevated plus maze (EPM). EPM is the most commonly employed animal behavioral model of anxiety. The test uses an elevated, plus-shaped (+) apparatus with two open and two enclosed arms.
The behavioral model is based on the general aversion of rodents to open spaces. Anxiety reduction is indicated in the plus-maze by an increase in the proportion of time spent in the open arms. In this study, rats were given either ethanol, diazepam (Valium), valerian root extract, valerenic acid, or a solution of valerenic acid and exogenous GABA, and assessed for the number of entries and time spent on the open arms of an elevated plus maze.
Results showed that there was a significant reduction in anxious behavior in valerian extract or valerenic acid exposed subjects compared to the ethanol control group.
Benke et al[19] also looked at the response of mice to valerenic acid and valerenol using EPM. In addition, they subjected the mice to the light-dark box test (LDB), another model used to assess anxiety in rodents. The LDB apparatus has two compartments. The light compartment is ⅔ of the box and is brightly lit and open. The dark compartment is ⅓ of the total box and is covered and dark. A door connects the two compartments.
Rodents prefer darker areas over lighter areas. However, when presented in a novel environment, rodents tend to explore. These two conflicting emotions lead to observable anxiety like symptoms.
In both tests, valerian decreased anxiety in the mice. Lastly, they repeated the experiments with a mutated mouse breed in which the area of the valerian-specific GABA receptor was absent. These mice did not show the same decrease in anxiety as the wild-type mice did.
Human studies: A 2015 study by Gharib et al [20] looked at the effect of valerian on women during an anxiety-provoking procedure. The subjects were 64 infertile women undergoing a hysterosalpingography (HSG)- a radiologic study of the uterus and fallopian tubes.
Women who received a single dose of valerian 30 minutes before the procedure were compared to women who received a placebo. The results revealed that women who received valerian had a significant decrease in their anxiety compared to those who received placebo.
Another study, by Ahmadi et al. [21] looked at the ability of valerian to moderate the anxiety producing side effect of efavirenz (EFV), an antiretroviral medication used in the treatment of HIV. Fifty-one HIV-positive patients were enrolled in a randomized, double-blinded, placebo-controlled, clinical trial. Patients received valerian (530 mg) or placebo nightly 1 hour before sleep for 4 weeks.
The neuropsychiatric status (sleep, anxiety, depression, suicidal thought, and psychosis) of patients was assessed at baseline and week 4 using validated questionnaires. Sleep and anxiety were significantly improved in the valerian group compared to the placebo group. The researchers concluded that valerian may be considered as a potential option in preventing neuropsychiatric adverse effects of efavirenz in HIV-positive patients.
Andreatini et al [22] looked at the effect on valerian extract on 36 patients with generalized anxiety disorder. The patients were divided into three groups- one received diazepam, another valerian extract, and the third a placebo. All patients were assessed at baseline and four weeks of treatment with two psychological tests- the State-Trait Anxiety Inventory (STAI) and the Hamilton Anxiety Rating Scale (HAM-A).
STAI is a psychological inventory consisting of 40 questions on a self-report basis. The STAI measures two types of anxiety - state anxiety, or anxiety about an event, and trait anxiety, or anxiety level as a personal characteristic. HAM-A is also a psychological questionnaire which looks at two groups of factors.
The psychic factor of HAM-A consists of anxious mood, tension, fears, cognitive or concentration disturbances, depressed mood, and behavior at interview. The somatic factor consists of insomnia and somatomuscular, somatosensory, cardiovascular, respiratory, gastrointestinal, genitourinary and autonomic symptoms.
The researchers found no significant differences between groups on total symptom scores, valerian appeared to be relatively more effective for psychic symptoms (on HAM-A subscores), while diazepam was better for STAI-trait anxiety.
Bottom Line
In vitro and in vivo studies support the concept that components of valerian extract can increase GABA levels in the central nervous system and that it acts at a specific site on GABA receptors. Clinical studies showing benefits of valerian are few in number and suggest it may work better for psychological symptoms than for trait anxiety.
Valerian did not reduce anxiety as well as benzodiazepines but might be considered for those who have undesirable side effects with traditional medical treatment.
Does It Lower Blood Pressure?
I could find no studies in PubMed about valerian effects on blood pressure.
Does it Ease Menstrual Cramps?

Although valerian has been traditionally used as a menstruating and sedative drug since 11th century, there is little scientific evidence to support this. There is only one paper in the scientific literature which looks at the effect of valerian on menstrual cramps. Mirabi et al[23] did a double-blind, randomized, placebo-controlled trial, in which 100 students were randomly assigned to receive valerian or placebo.
Valerian was given 3 times daily for 3 days beginning at the onset of menstruation, for 2 consecutive menstrual cycles. At baseline and during the intervention cycles, the pain severity and systemic manifestations were evaluated.
After the intervention, the pain severity was significantly reduced in both groups (P < 0.001), but the extent of the reduction was larger in the valerian group, with the difference between the 2 groups being statistically significant (P < 0.05). Scores of systemic manifestations associated with dysmenorrhea decreased after the intervention, but there was no significant difference between the groups.
Bottom line
There is insufficient evidence at this time to support the assertion that valerian eases menstrual cramps. Additional studies are needed.
Does It Improve Stress Management?

As the chief inhibitory neurotransmitter of the central nervous system, GABA is known to slow down neuron activity. According to Luscher et al[24], there is abundant evidence that GABA plays a prominent role in the brain control of stress.
As discussed above in the sleep and anxiety sections, valerian extracts may increase the release of GABA and decrease its re-uptake in neurons. Therefore, it seems reasonable that valerian could potentially be of benefit in relieving stress.
Unfortunately, there is little in the scientific literature that specifically looks at valerian for stress relief, especially in human subjects.
Jung et al.[25, 26] did two studies on the effect of valerenic acid (VA) in mice subjected to stressful conditions. In the first study, mice were given VA for three weeks before being subjected to physical or psychological stress. They looked at the responses by using a forced swim test (Mice are placed in an inescapable transparent tank that is filled with water and their escape related mobility behavior is measured) and by checking blood levels of corticosteroids, norepinephrine, serotonin, and their metabolites.
In the control group, immobility time and corticosteroid levels were significantly increased. These parameters were significantly decreased in mice that received VA. In addition, levels of the metabolites MHPG-SO4 and 5-HIAA were increase in the hippocampus and amygdala (respectively) of the mice brains. Fear and anxiety are believed to be mediated in these are areas of the brain.
Similar results were obtained in their second study [26] which looked at optimal VA dosing and the effect of VA on neurotransmitters in the hippocampus-amygdala region.
In clinical trials, a 1988 single-dose, double blind, placebo controlled study by Kohnen and Oswald [27] looked at the effect of valerian extract on performance and mood of healthy volunteers under social stress conditions. The volunteers were called up to solve mental arithmetic problems. Those taking valerian subjectively felt less anxious than controls and did not experience any sedation.
Cropley [28] looked at 54 participants who performed standardized word mental stress tasks on two occasions 1 week apart. Blood pressure (BP), heart rate (HR) and subjective ratings of pressure were assessed at rest and during the mental stress task. Half of the subjects then received kava or valerian for 7 days, while the rest acted as controls.
At a second session there was a significant decrease in systolic BP in the valerian and kava groups, but no decrease in diastolic BP. HR reaction to stress decreased in the valerian, but not the kava group. Individuals in both valerian and kava groups reported less pressure during the second task compared to the first time. Performance on the tasks did not change.
Kennedy et al [28] looked at a combination of valerian and Melissa officinalis (lemon balm). In this double-blind, placebo-controlled, randomized, balanced cross-over experiment, 24 healthy volunteers received three separate single doses (600 mg, 1200 mg, 1800 mg) of a standardized product containing M. officinalis and V. officinalis extracts, plus a placebo, on separate days separated by a 7 day wash out period.
Changes of mood and anxiety were assessed during pre-dose and 1 h, 3 h and 6 h post-dose completions of a Defined Intensity Stressor Simulation (DISS) battery.
Cognitive performance was also assessed. The results showed that the 600 mg dose of the combination decrease the negative effects of anxiety on the DISS battery. In addition, all three doses led to decreases in performance on the Stroop task module (a demonstration of interference in the reaction time of a task), and the two lower doses led to decreases on the overall score generated on the DISS battery.
Bottom line
Although, in theory, valerian could have a positive effect on stress, there is just insufficient scientific evidence at this time to recommend it.
Is Valerian Root (and or Supplementation) Safe?
Valerian is likely safe for most people when used in medicinal amounts for short periods of time. Clinical studies have reported safe use of valerian for medicinal purposes in over 12,000 people in trials lasting up to 28 days. The safety of long-term use is unknown. Some information suggests that valerian might also be safe when taken by children for 4-8 weeks.
Valerian can cause some side effects such as headache, excitability, dizziness, nausea, abdominal cramps and even insomnia in some people.
A few people feel sluggish in the morning after taking valerian, especially at higher doses. It’s best not to drive or operate dangerous machinery after taking valerian. Valerian may not be safe if you're pregnant or breast-feeding. And it has not been evaluated to determine if it's safe for children under 3 years old.
The long-term safety of valerian is unknown. To avoid possible side effects when discontinuing valerian after long-term use, it's best to reduce the dose slowly over a week or two before stopping completely.
Drug interactions are possible. Valerian may increase the effects of other sleep aids. It also increases the sedative effect of depressants, such as alcohol, benzodiazepines and narcotics. Valerian can interfere with some prescription medications. And it may interact with other dietary supplements, such as St. John's wort.
Conclusion
Valerian has been safely used for many years as a treatment for sleep disturbances and anxiety. In vitro and animal studies have shown that components of valerian extract, most notably valerenic acid, do have an effect on GABA receptors and GABA concentrations in brain tissue.
This biological activity has underpinned studies seeking herbal remedies for the treatment of sleep disorders, anxiety and stress-related illnesses.
Unfortunately, very few human studies are available to assess its efficacy, and those available are plagued by their small size and reliance on subjective measures of success or failure. There is also a lack of standardization of the form of valerian used. In addition, valerian is often combined with other herbs with similar traditional uses making it impossible to assess the ability of valerian extract alone to account for experimental results.
For anyone thinking of using valerian root to treat a specific health condition, it would prudent to discuss it with a health care professional before starting.

Leave a Reply